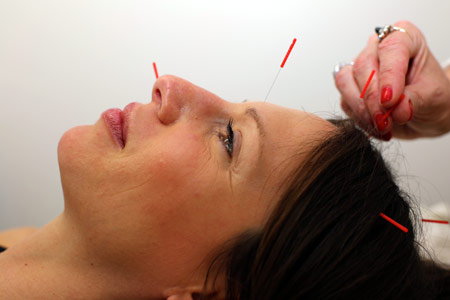
Acupuncture Chemotherapy Neuropathy Relief
Acupuncture alleviates neuropathic symptoms due to chemotherapy-induced peripheral neuropathy (CIPN) in breast cancer survivors. A randomized-controlled trial was conducted at the Dana-Farber Cancer Institute (Boston, Massachusetts). The results demonstrate that an 8-week intensive acupuncture protocol (18 sessions) greatly reduces pain intensity levels, pain interference, and average pain levels. [1] The results also show significant improvements in CIPN-specific and general quality of life scores, functional assessment of cancer therapy neurotoxicity subscales, and brief pain inventory short-form scores. In addition, stage I–III breast cancer patients with persistent CIPN after chemotherapy had better neurotoxicity questionnaire sensory scores (PNQ) over waitlist control patients. Moreover, low intensity acupuncture treatment regimens contributed to clinically significant reductions in sensory CIPN symptoms.
For the first week, researchers inserted acupuncture needles (0.20 × 25 mm and 0.25 × 40 mm) into specified main points to obtain the deqi sensation. From the second week to the eighth week, electroacupuncture was applied to TB5 (Waiguan) and Baxie (second) or SP6 (Sanyinjiao) and LR3 (Taichong), bilaterally. Acupoints were applied according to locations of CIPN symptoms, using alternating 2–10 Hz for 30 minutes each session. If the patients were very comfortable with acupuncture, researchers added Ex-LE12 (Qiduan) as a treatment point. Secondary treatment points included Ex-LE10 (Bafeng), LI11(Quchi), ST36 (Zusanli), SP9 (Yinlingquan), K3 (Taixi), and Yintang.
Chemotherapy drugs like Taxanes and platinum agents (especially paclitaxel and docetaxel) are widely used in the early stage and metastatic stages of breast cancer treatment, which can cause CIPN. The symptoms of CIPN vary, but usually present with pain and paresthesia. The incidence of CIPN in patients with breast cancer ranges between 30% and 97%, which is related with poor physical function, increased risk of falling, and greater disability in cancer survivors.
Many studies focus on medications or dietary supplements to treat CIPN in patients with cancer, including pharmacologic agents like duloxetine, antidepressants, anticonvulsants, non-narcotic and narcotic analgesics, or dietary supplements like glutamine, glutathione, vitamin E, and vitamin B12. Many treatments cause different types of side effects such as fatigue, dizziness, insomnia, and nausea.
Acupuncture is proven to be safe and demonstrates efficacy in alleviation of CIPN symptoms, improving nerve system conduction, and reducing symptom distress. [2–5] Importantly, acupuncture effectively prevents deterioration of CIPN from grade II to grade III in breast cancer patients after finishing paclitaxel chemotherapy. [7]
References:
[1]Weidong Lu, Anita Giobbie‐Hurder, Rachel A. Freedman, Im Hee Shin, Nancy U. Lin, Ann H. Partridge, David S. Rosenthal, and Jennifer A. Ligibel. Acupuncture for Chemotherapy–Induced Peripheral Neuropathy in Breast Cancer Survivors: A Randomized Controlled Pilot Trial. The Oncologist 2020;25:310–318.
[2]11. Bao T, Seidman AD, Piulson L et al. A phase IIa trial of acupuncture to reduce chemotherapy-induced peripheral neuropathy severity during neoadjuvant or adjuvant weekly paclitaxel chemotherapy in breast cancer patients. Eur J Cancer 2018;101:12–19.
[3] Garcia MK, Cohen L, Guo Y et al. Electroacupuncture for thalidomide/bortezomib-induced peripheral neuropathy in multiple myeloma: A feasibility study. J Hematol Oncol 2014;7:41.
[4] Molassiotis A, Suen LKP, Cheng HL et al. A randomized assessor-blinded wait-list-controlled trial to assess the effectiveness of acupuncture in the management of chemotherapy-induced peripheral neuropathy. Integr Cancer Ther 2019; 18:1534735419836501.
[5] Han X, Wang L, Shi H et al. Acupuncture combined with methylcobalamin for the treatment
of chemotherapy-induced peripheral neuropathy in patients with multiple myeloma. BMC Cancer 2017;17:40.
[6]Xu WR, Hua BJ, Hou W et al. Clinical randomized controlled study on acupuncture for treatment of peripheral neuropathy induced by chemotherapeutic drugs [in Chinese]. Zhong guo Zhen Jiu 2010;30:457–460.
[7]11. Bao T, Seidman AD, Piulson L et al. A phase IIa trial of acupuncture to reduce chemotherapy-induced peripheral neuropathy severity during neoadjuvant or adjuvant weekly paclitaxel chemotherapy in breast cancer patients. Eur J Cancer 2018;101:12–19.




 October is Breast Cancer Awareness month. My grandmother passed away from breast cancer at the age of 35 ( when my mom was only 3 month old) . My mom passed away from breast cancer at the age of 62….so now you can understand why 60 % of my practice is Breast Cancer Patients!! Why my mission in life is to fight for survival of these Women!!
October is Breast Cancer Awareness month. My grandmother passed away from breast cancer at the age of 35 ( when my mom was only 3 month old) . My mom passed away from breast cancer at the age of 62….so now you can understand why 60 % of my practice is Breast Cancer Patients!! Why my mission in life is to fight for survival of these Women!! SJ was referred to my practice for the 1st time in December 2018 by her
SJ was referred to my practice for the 1st time in December 2018 by her  “Going to Hollywood to talk about menopause
“Going to Hollywood to talk about menopause The Dao Masters believed that the key to a happy life is the balancing act of Yin and Yang within yourself. This individual balance centers you and makes it possible to strike a balance with another person ! What is Yin? It is a feminine, receiving, cooling, moistening-Moon Energy 🌙. What is Yang? It is male, proactive, giving, doing, achieving, warming, activating, initiating- the energy of the Sun 🌞! So….. we are all responsible for being centered and balanced within yourself and only then can we have happy and healthy sexual relationships with our partners 💥💫✨🔥 We are in a New Moon Phase of Lunar calendar right now, which is Yin. It requires the most Yin nourishment… herbal and acupuncture. Read about it in my chapter in the Textbook of Clinical Sexual Medicine published by Springer International in 2017 or please come to visit me or give me a call at 310-444-6212 to find more about it…🌔#moon #moonlight #yinyang #male #female #balance #sexualbalance #love #healthysexy #healingjourney #acupuncture #lucypostolov #waguihsiag
The Dao Masters believed that the key to a happy life is the balancing act of Yin and Yang within yourself. This individual balance centers you and makes it possible to strike a balance with another person ! What is Yin? It is a feminine, receiving, cooling, moistening-Moon Energy 🌙. What is Yang? It is male, proactive, giving, doing, achieving, warming, activating, initiating- the energy of the Sun 🌞! So….. we are all responsible for being centered and balanced within yourself and only then can we have happy and healthy sexual relationships with our partners 💥💫✨🔥 We are in a New Moon Phase of Lunar calendar right now, which is Yin. It requires the most Yin nourishment… herbal and acupuncture. Read about it in my chapter in the Textbook of Clinical Sexual Medicine published by Springer International in 2017 or please come to visit me or give me a call at 310-444-6212 to find more about it…🌔#moon #moonlight #yinyang #male #female #balance #sexualbalance #love #healthysexy #healingjourney #acupuncture #lucypostolov #waguihsiag